Halifax police in a ‘state of crisis’ following rising mental health claims
Posted Apr 10, 2022 07:15:00 PM.
A Halifax advocate for police officers wants better local resources and treatment options to prevent mental health crises among first responders.
“I don't think it's any secret that it would be accurate to describe the police department right now as in a state of crisis in terms of our ability to deliver a service,” Dean Stienburg, president of the Halifax Regional Police Association, said. “That comes down to a lack of person power.
“A big part of that is the fact that we've seen a very large increase in the number of mental health injuries that our officers are experiencing.”
Over the past several years, the number of Halifax Regional Police officers making mental health claims has steadily increased. That number drastically rose starting in January 2020.
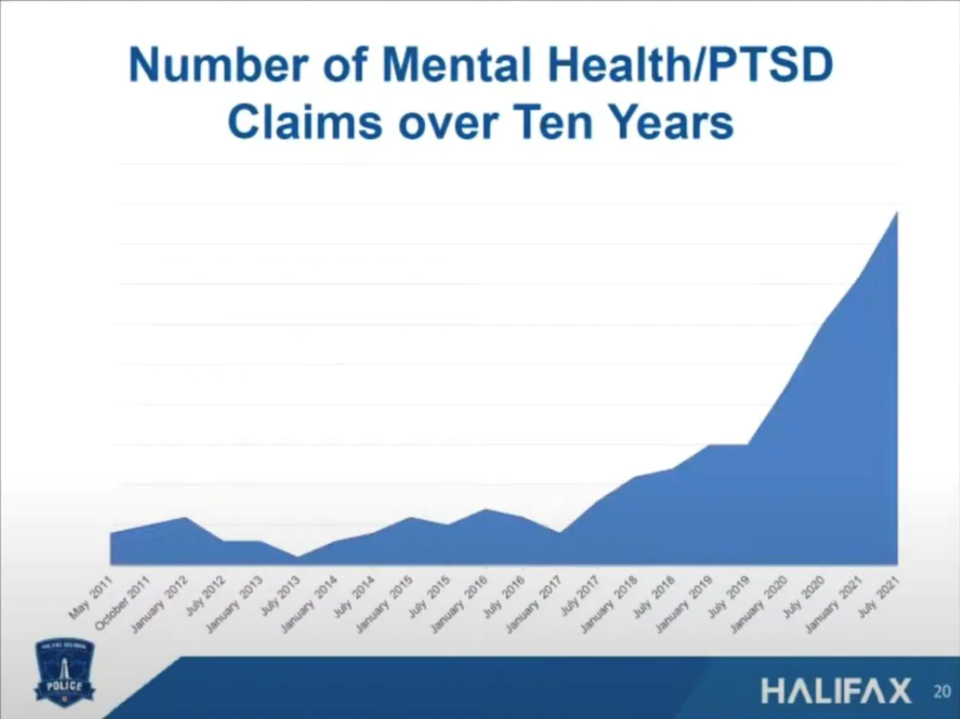
While the COVID-19 pandemic has impacted the mental health of many, Stienburg told The Todd Veinotte Show people can't pinpoint the recent rise in mental health claims by officers to one specific reason.
“Like most crises, they occur because you've got a number of factors that happen,” Stienburg, who's been an officer for more than 30 years, said. “Did the pandemic play a role? Absolutely. Are there other factors that play a role? Yes. Do the officers need more support on pretty much every level and more resources for what they do? Yes.
“That's something we can debate, and we'll probably debate long after this [pandemic] is over.”
But at the moment, Stienburg said he wants to focus on other problems.
“I think the more pressing question, right now, is, 'What do we do fix it?'” he said. “'How do we get these officers healthy again and get them back to work and being able to contribute in a meaningful way?' That's really what their desire is.
“That's our biggest challenge right now and that's what needs to be focused on.”
Earlier this month, the Board of Police Commissioners directed municipal staff to study the causes of more officers making mental health claims along with any possible solutions.
Stienburg said he thinks it's a step in the right direction since finding the reason will hopefully help prevent a similar crisis from occurring in the future.
“But I don't know that the study is going to necessarily affect things in the short term,” he said. “I think that's probably more pressing, is getting people healthy again. Then, we can definitely take a long look at what got us here and try and avoid those pitfalls in the future.”
Currently, he said the current health care system isn't set up to effectively help these officers and other first responders across Canada.
“Our system's not in a position to be able to provide the intensive therapy and treatment that they need — and the early detection that's required — in order to prevent officers from ending up being so sick that they have to go off work,” Stienburg said.
While early detection is part of the problem according to Stienburg, treatment is slow once an illness is diagnosed. For instance, he said a patient might get a diagnosis, get an appointment six weeks later and then possibly see gradual treatment every following week.
Stienburg said there are more intensive programs available, but they're typically outside of Nova Scotia and quite costly.
Going forward, he said the focus must be on figuring out how to solve the issue while working with the government and stakeholders to get treatment facilities and proper treatment for first responders here in Nova Scotia.
“It's fine to send them to Ontario, and these are great facilities that do great work,” Stienburg said. “But then when they come back, there's no follow-up support.
“We really do need something in the province to service everyone's needs in the first responder community.”